Vaginismus is likely a medical term you may not have heard of. Yet this condition is thought to affect between 1-17% of women worldwide, and between 12-21% in North America.
Also known as “Genito pelvic pain penetration disorder”, this disorder is often embarrassing or uncomfortable for many women to discuss, adding to a lack of education and treatment surrounding the condition.
If you have difficulty, pain or discomfort with vaginal penetration, be it related to inserting a tampon, medical examinations, sexual devices or intercourse, you may have questions about whether or not you too may be suffering from vaginismus.
Before we dive into the signs and symptoms of vaginismus, let’s briefly delve into what this condition is and the potential causes.
45-Min Online Pelvic Therapy Session, $99 
What is Vaginismus?
This medical condition involves involuntary muscle contractions, spasms and cramping of the pelvic floor. This may feel like a tightening, cramp, pressure or pain.
These involuntary contractions are typically associated with a stimulus (either psychological or physical), such as an anxiety or trauma response to sexual penetration, or simply an involuntary non-psychological response to pressure or touch in that area.
This can make sexual intercourse, use of tampons, or even a gynecological exam painful or even impossible.
The most typical muscle group affected by this condition include the pubococcygeus (PC) musculature (responsible for orgasms, intercourse, bowel movements, urination and childbirth).
Quick Facts About Vaginismus
- The condition can get worse over time, but is treatable
- The condition is non-contagious and involuntary (not your fault)
- Symptoms, severity and type can vary per individual
- Vaginismus can result from medical as well as psychological factors
- Treatment can be highly effective for many women
Do I Have Vaginismus?
Although only a medical professional can officially diagnose you with Vaginismus, there are several key symptoms that may indicate you are afflicted with this condition. If you experience any of these, evaluation by a licensed medical professional is advisable.
Just know that the condition, although difficult to talk about, is more common than you think, and you’re not alone. Your body is sending you signals for a reason. Listen to it and you’ll be one step closer to overcoming any challenges you are experiencing.
What Does Vaginismus Feel Like?
Vaginismus can feel like a sharp or burning pain at the entrance of the vagina, often accompanied by a sensation of tightness or pressure. This involuntary contraction of the vaginal muscles makes penetration, whether by a tampon, a medical instrument, or a penis, extremely uncomfortable or impossible.
Types of Vaginismus
1. Primary
Also known as “lifelong vaginismus” those with the primary type experience pain and/or discomfort every time anything has penetrated (or attempted to have penetrated) the vagina.
Those with the primary type have dealt with the condition their whole lives. Often it is first experienced when trying to use a tampon, attempting intercourse for the first time, or the first time a pelvic examination is attempted by a doctor.
2. Secondary
Those with secondary vaginismus have achieved penetration without pain in the past. A life event, change in medical status, new health condition, or life stress may occur that brings about difficulty with penetration.
People with this form of vaginismus but may experience pain or difficulty after penetration or only on occasion as well.
What are the Signs and Symptoms of Vaginismus?
The leading sign of vaginismus is dyspareunia (painful sex), and is often the first indication of a problem. Although the pain associated with intercourse typically goes away after penetration (or attempted penetration) is over, that is not always the case.
Many women describe the pain as a burning, pressure, or like the penis has run into a block. Women with vaginismus can also experience bleeding. But discomfort is not limited to sexual intercourse. Pain or discomfort with the use of a tampon or during pelvic exams is common.
Other Common Symptoms Include:
- Inability to insert a tampon
- Inability to insert a sex toy or device
- Fear or pain associated with sexual activity
- Loss of sexual desire or performance anxiety
- Random muscle spasms of the pelvic area or wall
- Triggered spasms from massage, foreplay, or oral stimulation
- Hypertonic pelvic floor: long, sustained contractions that are uncomfortable or painful
- Tension in hips, hamstrings, low back, and abdominal muscles
Symptoms can range from mild to severe, are involuntary, and generally do not get better without intervention or treatment.
Vaginismus can result in serious emotional and psychological distress, impacting quality of life and making it difficult to maintain healthy sexual relationships.
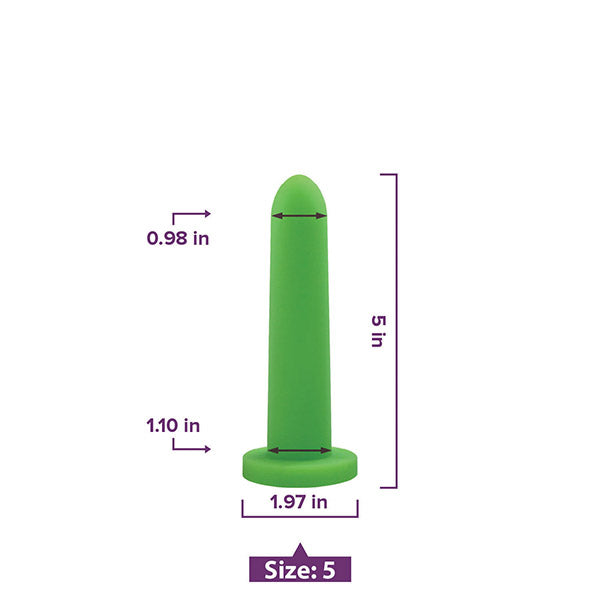
How does a vaginal dilator work?
What Can You Do if You Think You May Have Vaginismus?
Far too many women choose to just ‘live with it’. Whether this is due to the taboo nature of the topic or embarrassment, you don’t have to suffer the same fate.
There are several highly effective and largely non-invasive treatment options to help. At Intimate Rose we have dedicated our lives to helping women overcome such challenges with safe, effective, affordable and discreet treatment options proven to improve health and well-being.
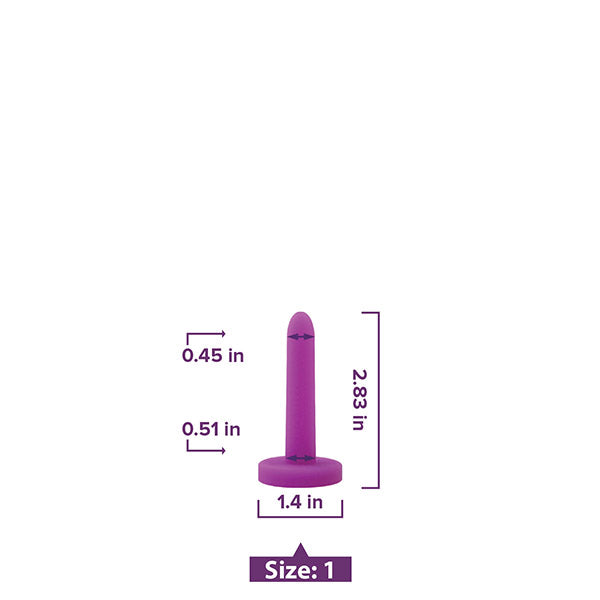
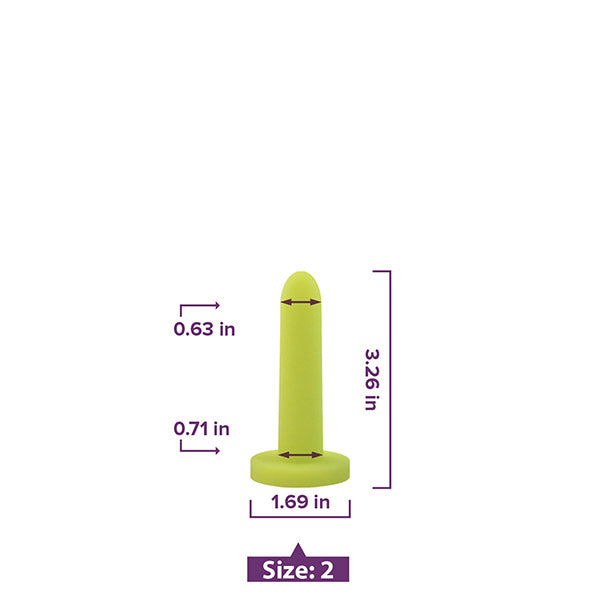
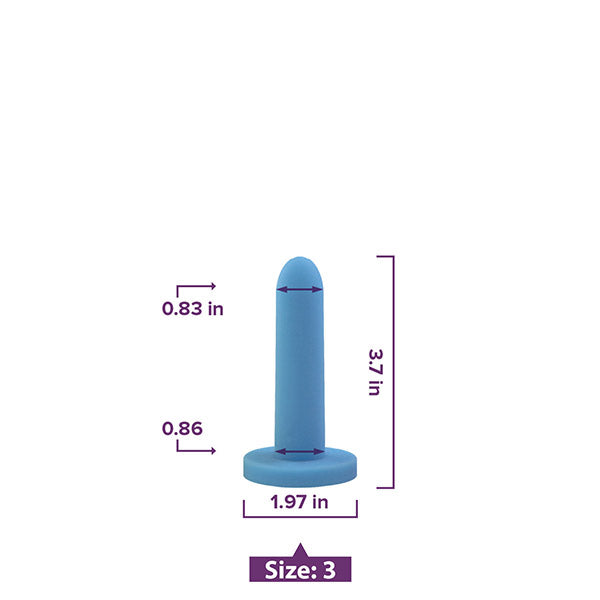
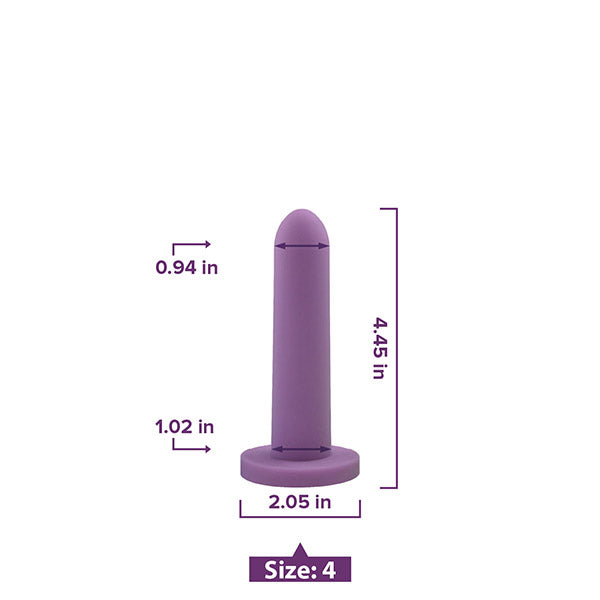
Something as simple as vaginal dilator therapy carried out in the comfort and privacy of your own home can yield incredible results.
If you suspect you may have Vaginismus, we always suggest a medical evaluation by a professional. Once you know what you’re dealing with, discuss the use of vaginal dilator therapy with your medical provider and reach out to our team for help getting the support you need.

45-Min Online Pelvic Therapy Session, $99