Periods are generally not a pleasant experience - so if you're experiencing pain when inserting a tampon, it makes an unpleasant experience even worse.
There are many underlying causes for pain when inserting a tampon. If you're currently experiencing this, do not force the tampon to go in; this may only cause more pain or damage to the interior walls of your vagina.
We've put together a review of some of the causes of tampon pains, your next steps in dealing with them, and when to see a doctor about them.
Vaginismus Or Tight Pelvic Muscles May Be the Cause
If it hurts when putting a tampon in, overly tight pelvic muscles as well as an involuntary condition known as vaginismus may be the reason. Occurring in anywhere between 5-17% of vagina owners, vaginismus is a condition that causes extreme pain or discomfort when inserting anything into the vagina--including insertion during intercourse or inserting tampons.
A 2010 review of vaginismus found that while some researchers attribute vaginismus to muscle spasms in the pelvic floor, this is hard to measure and is not always the case (Lahaie et al).
Vaginismus has a reciprocal relationship with anxiety; fear of insertion (which is sometimes due to negative attitudes about sex and vaginas or sexual trauma) can cause pain upon insertion, and the pain can reinforce and exacerbate the fear response (Lahaie et al).
Because of its reciprocal relationship with anxiety, psychotherapy and relaxation techniques may help reduce pain with vaginismus.
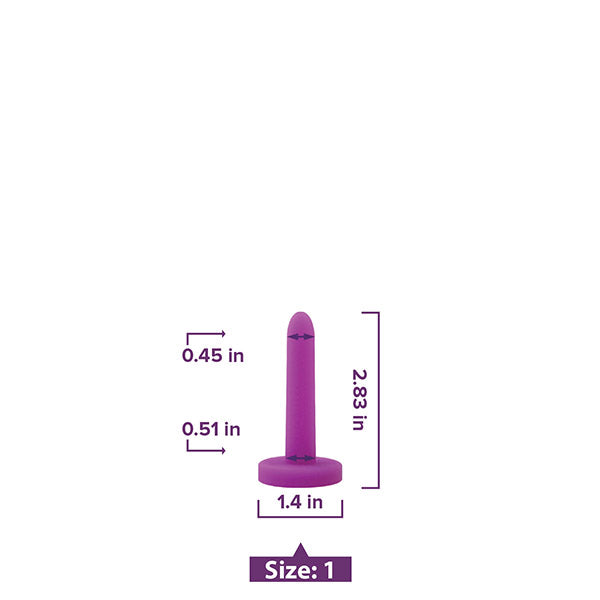
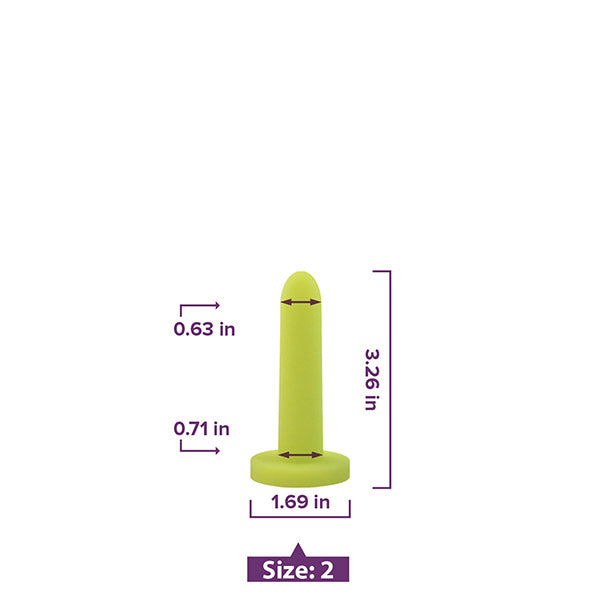
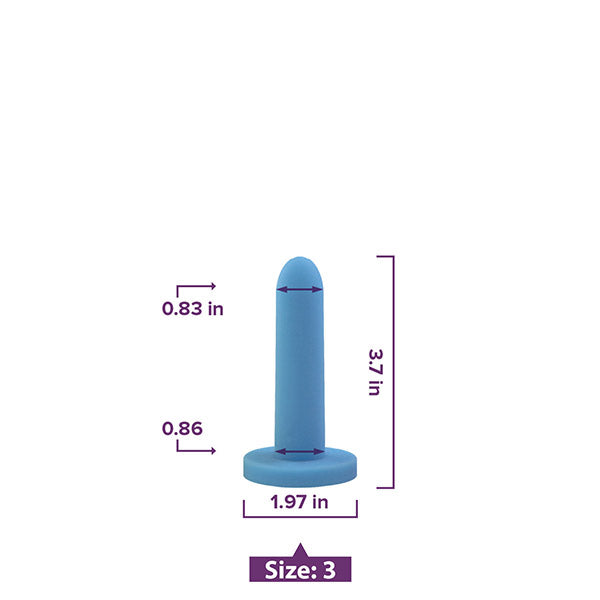
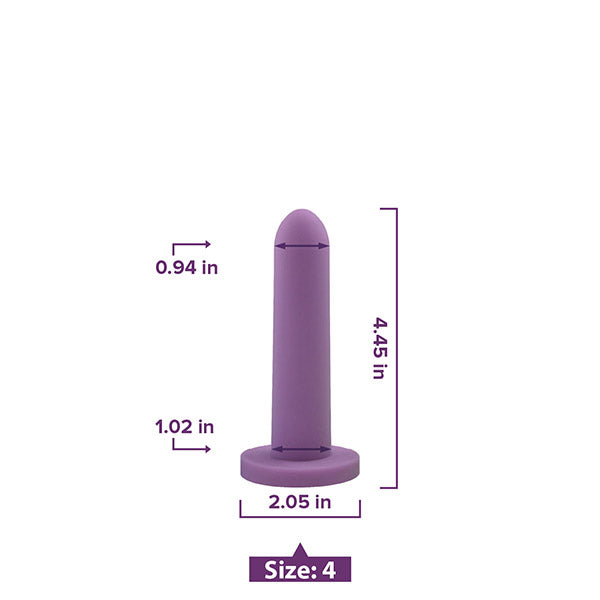
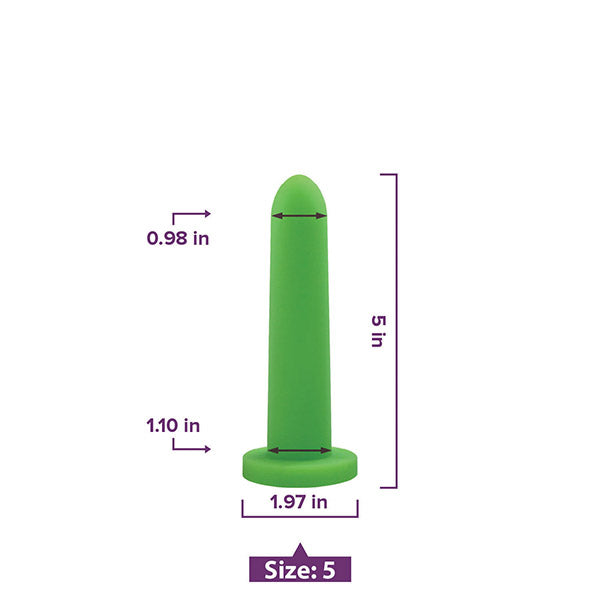
Vaginal trainers (also known as vaginal dilators) are also a very common treatment option for those with vaginismus or other kinds of vaginal pain.
In a small study from 2013, 31 out of 35 women studied had significant improvements in their vaginal pain upon insertion by using a combination of therapy and vaginal dilation (ter Kuile et al).
Vaginismus can be a painful and distressing condition, but it is treatable. If you experience pain when inserting a tampon, during intercourse, or when inserting other sexual stimuli, talk to your doctor or gynecologist.

45-Min Online Pelvic Therapy Session, $99
Painful Tampon Insertion from Vaginitis
Vaginitis is a common short-term condition, caused by an infection (including a yeast infection) or other changes in the bacteria of your vagina.
Vaginitis can be a symptom of the sexually transmitted infection Trichomoniasis, otherwise known as Trich (pronounced "Trick"). This STI is very common; the World Health Organization estimated about 248 million cases in 2005.
The drug Metronidazole has been shown to be about 95% effective in treating trichomoniasis (Cudmore et al, 2004).
Most types of vaginitis will be accompanied by pain, itching, and/or abnormal discharge. If your discharge is thick and lumpy (some compare it to cottage cheese), you may have a yeast infection; if it is yellow or green and has an unpleasant smell, it may be trichomoniasis (Spence & Melville, 2007).
Whatever the cause of your vaginitis, talk to your doctor as soon as you can; most vaginal infections or imbalances of bacteria can be quickly and safely resolved.
How does a vaginal dilator work?
Painful Insertion Due to Vaginal dryness
If your vagina is too dry when trying to insert a tampon, it may cause friction and pain inside your vagina.
Sometimes this is simply the result of a lighter flow of menstrual blood, possibly toward the end of your period; if that's the case, you may want to switch to a smaller tampon or use a pad.
However, if your vaginal dryness is chronic, there are many things that might be causing it. It could be due to stress, hormones, changes in medication, or douching.
If your vaginal dryness lasts more than a few days, talk to your doctor.
Conclusion
There are many reasons why you might be experiencing pain when inserting a tampon, but all of them have a solution and most are not serious. The cause of your pain can be answered by looking at related symptoms:
- Are you experiencing vaginal dryness? If so, use a smaller tampon or a pad for now, and talk to your doctor if the problem persists.
- Is your vaginal discharge abnormal (yellow or green, thick and lumpy, or malodorous)? If so, you may have vaginitis caused by a yeast infection or an STD. Vaginitis is generally not serious and quickly treatable; see a doctor as soon as you can.
- Do you experience pain when trying to put anything in your vagina? You may need to talk to your doctor about vaginismus and come up with a plan to treat it.
References
- Lahaie, M. A., Boyer, S. C., Amsel, R., Khalifé, S., & Binik, Y. M. (2010). Vaginismus: a review of the literature on the classification/diagnosis, etiology and treatment. Women's health (London, England), 6(5), 705–719. https://doi.org/10.2217/whe.10.46
- ter Kuile, M. M., Melles, R., de Groot, H. E., Tuijnman-Raasveld, C. C., & van Lankveld, J. J. (2013). Therapist-aided exposure for women with lifelong vaginismus: A randomized waiting-list control trial of efficacy. Journal of consulting and clinical psychology, 81(6), 1127. https://doi.org/10.1037/a0014273
- World Health Organization. (2011). Prevalence and incidence of selected sexually transmitted infections, Chlamydia trachomatis, Neisseria gonorrhoeae, syphilis and Trichomonas vaginalis: methods and results used by WHO to generate 2005 estimates (No. Chlamydia infections).
- Cudmore, S. L., Delgaty, K. L., Hayward-McClelland, S. F., Petrin, D. P., & Garber, G. E. (2004). Treatment of infections caused by metronidazole-resistant Trichomonas vaginalis. Clinical microbiology reviews, 17(4), 783-793.
- Spence, D., & Melville, C. (2007). Vaginal discharge. BMJ (Clinical research ed.), 335(7630), 1147–1151. https://doi.org/10.1136/bmj.39378.633287.80

45-Min Online Pelvic Therapy Session, $99