If you have ever experienced pain before, during, or after sexual intercourse, you are far from being alone. According to the American College of Obstetricians and Gynecologists (ACOG), as many as 3 out of 4 women will experience painful sex in their lifetimes (ACOG, 2018).
For some women, this painful intercourse, which is called dyspareunia, is a temporary ailment. For others, it can persist over time and can take a toll on sexual health, relationships, and quality of life.
Fortunately, dyspareunia does not have to be a life-long condition and many at-home treatment options exist for women.
What Causes Dyspareunia?
As mentioned, dyspareunia describes pain in the pelvic or genital area with sexual intercourse and can occur before, during, or after intercourse. Some women experience pain with any penetration of the vagina, including when using a tampon or undergoing a pelvic exam with a speculum.
Some common causes of dyspareunia include:
- Vaginal trauma or injury due to childbirth, pelvic surgery, episiotomy, or radiation
- Vaginal dryness from menopause, medications, childbirth, breastfeeding, or low arousal
- Skin or vaginal infections such as yeast or urinary tract infections
- Pelvic conditions such as interstitial cystitis, pelvic inflammatory disease, or endometriosis
- Tight or spasming muscles of the pelvic floor
The pelvic floor muscles, which form a sling-like structure in the lower pelvis, support the pelvic organs and surround the vaginal wall. As with other muscles, these muscles can become tight and develop painful knots.
Pelvic floor tightness can have physical causes such as injury or poor posture, but it can also be caused by emotional issues such as stress, poor self-image, fear of intimacy, or sexual abuse. These factors can cause unconscious tensing and clenching of the pelvic floor, leading to difficult and painful intercourse.
45-Min Online Pelvic Therapy Session, $99 
Home Remedies for Dyspareunia
In most cases, dyspareunia can be treated with consistent use of at-home treatment options. A pelvic floor physical therapist can also help you get started with some of these techniques. Often, it is a combination of the strategies below that provide the best results.
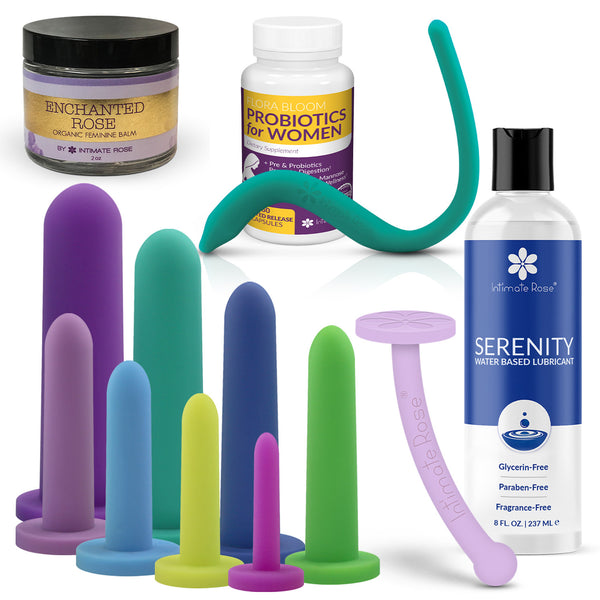
1. Lubricants
When vaginal dryness is a cause of painful sex, using lubricants can be extremely helpful. If you are using a condom, water-soluble or silicone-based lubricants are the best choice, since they will not break down the condom.
2. Vaginal Dilators
For pelvic floor tightness causes by involuntary muscles spasms, vaginal dilators are specific tools in a variety of sizes that allow you to gradually stretch and release the pelvic floor muscles and are best used with the guidance of a pelvic physical therapist. The Intimate Rose Vaginal Dilators are cleared to treat the symptoms of Vaginismus such as painful intercourse, known as dyspareunia.
Dilators, which are often made out of silicone for comfort, are a gentle way to train the brain and the muscles of the pelvic floor to relax during insertion. Dilator therapy is best performed in combination with relaxed breathing, which encourages the muscles of the pelvic floor to open up and relax.
It can also be helpful to use visualization while using the dilator, picturing the pelvic floor opening up like a flower.
3. Pelvic Floor Wands
Tension in the muscles of the pelvic floor can cause pain at rest and during sex. To relieve these aches and pains, a specially designed pelvic floor therapy wand, such as Intimate Rose’s exclusively patented Pelvic Wand, can be used either vaginally or rectally to access these hard-to-reach muscles.
When you move the wand around the pelvic floor, areas of tension can be identified as particularly sensitive spots. By applying gentle pressure to these areas for 1-2 minutes, the muscles can relax. This should be done daily
How does a vaginal dilator work?
4. Breathing Exercises
Because of the structure of the abdominal wall, the muscles of the pelvic floor can be influenced by our breathing patterns. By practicing relaxed breathing in a quiet place, preferably laying down, the pelvic floor can be gently mobilized and stretched.
With each inhale, the pelvic floor drops slightly, providing a gentle stretch to the muscles. With each exhale, the pelvic floor returns to its resting position. It can be helpful to place your hand along the perineum to help feel the slight drop of the pelvic floor with inhalation, providing additional feedback to the brain.
5. Pelvic Release Exercises
The muscles of the pelvic floor can be stretched gently with exercises that open up the hip, many of which are common yoga poses. Combined with relaxed breathing, these exercises can help you learn to consciously release the pelvic floor muscles and retrain your body to let go of unconscious tension.
With the right tools and consistent practice, sex can become pain-free and enjoyable once again.
References:
American College of Obstetricians and Gynecologists. (2018). When Sex is Painful. https://www.acog.org/womens-health/faqs/when-sex-is-painful?utm_source=redirect&utm_medium=web&utm_campaign=otn

45-Min Online Pelvic Therapy Session, $99